Oncology
Citation Information: J Clin Invest. 2012. https://doi.org/10.1172/JCI62229.
Abstract
Epithelial ovarian cancers (EOCs) often exhibit morphologic features of embryonic Müllerian duct–derived tissue lineages and colonize peritoneal surfaces that overlie connective and adipose tissues. However, the mechanisms that enable EOC cells to readily adapt to the peritoneal environment are poorly understood. In this study, we show that expression of HOXA9, a Müllerian-patterning gene, is strongly associated with poor outcomes in patients with EOC and in mouse xenograft models of EOC. Whereas HOXA9 promoted EOC growth in vivo, HOXA9 did not stimulate autonomous tumor cell growth in vitro. On the other hand, expression of HOXA9 in EOC cells induced normal peritoneal fibroblasts to express markers of cancer-associated fibroblasts (CAFs) and to stimulate growth of EOC and endothelial cells. Similarly, expression of HOXA9 in EOC cells induced normal adipose- and bone marrow–derived mesenchymal stem cells (MSCs) to acquire features of CAFs. These effects of HOXA9 were due in substantial part to its transcriptional activation of the gene encoding TGF-β2 that acted in a paracrine manner on peritoneal fibroblasts and MSCs to induce CXCL12, IL-6, and VEGF-A expression. These results indicate that HOXA9 expression in EOC cells promotes a microenvironment that is permissive for tumor growth.
Authors
Song Yi Ko, Nicolas Barengo, Andras Ladanyi, Ju-Seog Lee, Frank Marini, Ernst Lengyel, Honami Naora
Citation Information: J Clin Invest. 2012. https://doi.org/10.1172/JCI61067.
Abstract
The chemokine receptor CXCR2 is a key mediator of neutrophil migration that also plays a role in tumor development. However, CXCR2 influences tumors through multiple mechanisms and might promote or inhibit tumor development depending on context. Here, we used several mouse models of spontaneous and inflammation-driven neoplasia to define indispensable roles for CXCR2 in benign and malignant tumors. CXCR2-activating chemokines were part of the secretome of cultured primary benign intestinal adenomas (ApcMin/+) and highly expressed by all tumors in all models. CXCR2 deficiency profoundly suppressed inflammation-driven tumorigenesis in skin and intestine as well as spontaneous adenocarcinoma formation in a model of invasive intestinal adenocarcinoma (AhCreER;Apcfl/+;Ptenfl/fl mice). Pepducin-mediated CXCR2 inhibition reduced tumorigenesis in ApcMin/+ mice. Ly6G+ neutrophils were the dominant source of CXCR2 in blood, and CXCR2 deficiency attenuated neutrophil recruitment. Moreover, systemic Ly6G+ cell depletion purged CXCR2-dependent tumor-associated leukocytes, suppressed established skin tumor growth and colitis-associated tumorigenesis, and reduced ApcMin/+ adenoma formation. CXCR2 is thus a potent protumorigenic chemokine receptor that directs recruitment of tumor-promoting leukocytes into tissues during tumor-inducing and tumor-driven inflammation. Similar leukocyte populations were also found in human intestinal adenomas, which suggests that CXCR2 antagonists may have therapeutic and prophylactic potential in the treatment of cancer.
Authors
Thomas Jamieson, Mairi Clarke, Colin W. Steele, Michael S. Samuel, Jens Neumann, Andreas Jung, David Huels, Michael F. Olson, Sudipto Das, Robert J.B. Nibbs, Owen J. Sansom
Citation Information: J Clin Invest. 2012. https://doi.org/10.1172/JCI62129.
Abstract
Cancer cells exhibit an aberrant metabolism that facilitates more efficient production of biomass and hence tumor growth and progression. However, the genetic cues modulating this metabolic switch remain largely undetermined. We identified a metabolic function for the promyelocytic leukemia (PML) gene, uncovering an unexpected role for this bona fide tumor suppressor in breast cancer cell survival. We found that PML acted as both a negative regulator of PPARγ coactivator 1A (PGC1A) acetylation and a potent activator of PPAR signaling and fatty acid oxidation. We further showed that PML promoted ATP production and inhibited anoikis. Importantly, PML expression allowed luminal filling in 3D basement membrane breast culture models, an effect that was reverted by the pharmacological inhibition of fatty acid oxidation. Additionally, immunohistochemical analysis of breast cancer biopsies revealed that PML was overexpressed in a subset of breast cancers and enriched in triple-negative cases. Indeed, PML expression in breast cancer correlated strikingly with reduced time to recurrence, a gene signature of poor prognosis, and activated PPAR signaling. These findings have important therapeutic implications, as PML and its key role in fatty acid oxidation metabolism are amenable to pharmacological suppression, a potential future mode of cancer prevention and treatment.
Authors
Arkaitz Carracedo, Dror Weiss, Amy K. Leliaert, Manoj Bhasin, Vincent C.J. de Boer, Gaelle Laurent, Andrew C. Adams, Maria Sundvall, Su Jung Song, Keisuke Ito, Lydia S. Finley, Ainara Egia, Towia Libermann, Zachary Gerhart-Hines, Pere Puigserver, Marcia C. Haigis, Elefteria Maratos-Flier, Andrea L. Richardson, Zachary T. Schafer, Pier P. Pandolfi
Citation Information: J Clin Invest. 2012. https://doi.org/10.1172/JCI62110.
Abstract
Chemotactic cytokines (chemokines) can help regulate tumor cell invasion and metastasis. Here, we show that chemokine 25 (CCL25) and its cognate receptor chemokine receptor 9 (CCR9) inhibit colorectal cancer (CRC) invasion and metastasis. We found that CCR9 protein expression levels were highest in colon adenomas and progressively decreased in invasive and metastatic CRCs. CCR9 was expressed in both primary tumor cell cultures and colon-cancer-initiating cell (CCIC) lines derived from early-stage CRCs but not from metastatic CRC. CCL25 stimulated cell proliferation by activating AKT signaling. In vivo, systemically injected CCR9+ early-stage CCICs led to the formation of orthotopic gastrointestinal xenograft tumors. Blocking CCR9 signaling inhibited CRC tumor formation in the native gastrointestinal CCL25+ microenvironment, while increasing extraintestinal tumor incidence. NOTCH signaling, which promotes CRC metastasis, increased extraintestinal tumor frequency by stimulating CCR9 proteasomal degradation. Overall, these data indicate that CCL25 and CCR9 regulate CRC progression and invasion and further demonstrate an appropriate in vivo experimental system to study CRC progression in the native colon microenvironment.
Authors
Huanhuan Joyce Chen, Robert Edwards, Serena Tucci, Pengcheng Bu, Jeff Milsom, Sang Lee, Winfried Edelmann, Zeynep H. Gümüs, Xiling Shen, Steven Lipkin
Citation Information: J Clin Invest. 2012. https://doi.org/10.1172/JCI61216.
Abstract
Crosstalk between the Notch and wingless-type MMTV integration site (WNT) signaling pathways has been investigated for many developmental processes. However, this negative correlation between Notch and WNT/β-catenin signaling activity has been studied primarily in normal developmental and physiological processes in which negative feedback loops for both signaling pathways are intact. We found that Notch1 signaling retained the capability of suppressing the expression of WNT target genes in colorectal cancers even when β-catenin destruction by the adenomatous polyposis coli (APC) complex was disabled. Activation of Notch1 converted high-grade adenoma into low-grade adenoma in an Apcmin mouse colon cancer model and suppressed the expression of WNT target genes in human colorectal cancer cells through epigenetic modification recruiting histone methyltransferase SET domain bifurcated 1 (SETDB1). Extensive microarray analysis of human colorectal cancers also showed a negative correlation between the Notch1 target gene, Notch-regulated ankyrin repeat protein 1 (NRARP), and WNT target genes. Notch is known to be a strong promoter of tumor initiation, but here we uncovered an unexpected suppressive role of Notch1 on WNT/β-catenin target genes involved in colorectal cancer.
Authors
Hyun-A Kim, Bon-Kyoung Koo, Ji-Hoon Cho, Yoon-Young Kim, Jinwoo Seong, Hee Jin Chang, Young Min Oh, Daniel E. Stange, Jae-Gahb Park, Daehee Hwang, Young-Yun Kong
Citation Information: J Clin Invest. 2012. https://doi.org/10.1172/JCI63608.
Abstract
Metastatic cancer is extremely difficult to treat, and the presence of metastases greatly reduces a cancer patient’s likelihood of long-term survival. The ZEB1 transcriptional repressor promotes metastasis through downregulation of microRNAs (miRs) that are strong inducers of epithelial differentiation and inhibitors of stem cell factors. Given that each miR can target multiple genes with diverse functions, we posited that the prometastatic network controlled by ZEB1 extends beyond these processes. We tested this hypothesis using a mouse model of human lung adenocarcinoma metastasis driven by ZEB1, human lung carcinoma cells, and human breast carcinoma cells. Transcriptional profiling studies revealed that ZEB1 controls the expression of numerous oncogenic and tumor-suppressive miRs, including miR-34a. Ectopic expression of miR-34a decreased tumor cell invasion and metastasis, inhibited the formation of promigratory cytoskeletal structures, suppressed activation of the RHO GTPase family, and regulated a gene expression signature enriched in cytoskeletal functions and predictive of outcome in human lung adenocarcinomas. We identified several miR-34a target genes, including Arhgap1, which encodes a RHO GTPase activating protein that was required for tumor cell invasion. These findings demonstrate that ZEB1 drives prometastatic actin cytoskeletal remodeling by downregulating miR-34a expression and provide a compelling rationale to develop miR-34a as a therapeutic agent in lung cancer patients.
Authors
Young-Ho Ahn, Don L. Gibbons, Deepavali Chakravarti, Chad J. Creighton, Zain H. Rizvi, Henry P. Adams, Alexander Pertsemlidis, Philip A. Gregory, Josephine A. Wright, Gregory J. Goodall, Elsa R. Flores, Jonathan M. Kurie
Citation Information: J Clin Invest. 2012. https://doi.org/10.1172/JCI62374.
Abstract
The DNA damage response (DDR) is a complex regulatory network that is critical for maintaining genome integrity. Posttranslational modifications are widely used to ensure strict spatiotemporal control of signal flow, but how the DDR responds to environmental cues, such as changes in ambient oxygen tension, remains poorly understood. We found that an essential component of the ATR/CHK1 signaling pathway, the human homolog of the Caenorhabditis elegans biological clock protein CLK-2 (HCLK2), associated with and was hydroxylated by prolyl hydroxylase domain protein 3 (PHD3). HCLK2 hydroxylation was necessary for its interaction with ATR and the subsequent activation of ATR/CHK1/p53. Inhibiting PHD3, either with the pan-hydroxylase inhibitor dimethyloxaloylglycine (DMOG) or through hypoxia, prevented activation of the ATR/CHK1/p53 pathway and decreased apoptosis induced by DNA damage. Consistent with these observations, we found that mice lacking PHD3 were resistant to the effects of ionizing radiation and had decreased thymic apoptosis, a biomarker of genomic integrity. Our identification of HCLK2 as a substrate of PHD3 reveals the mechanism through which hypoxia inhibits the DDR, suggesting hydroxylation of HCLK2 is a potential therapeutic target for regulating the ATR/CHK1/p53 pathway.
Authors
Liang Xie, Xinchun Pi, Ashutosh Mishra, Guohua Fong, Junmin Peng, Cam Patterson
Citation Information: J Clin Invest. 2012. https://doi.org/10.1172/JCI43354.
Abstract
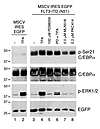
Mutations that activate the fms-like tyrosine kinase 3 (FLT3) receptor are among the most prevalent mutations in acute myeloid leukemias. The oncogenic role of FLT3 mutants has been attributed to the abnormal activation of several downstream signaling pathways, such as STAT3, STAT5, ERK1/2, and AKT. Here, we discovered that the cyclin-dependent kinase 1 (CDK1) pathway is also affected by internal tandem duplication mutations in FLT3. Moreover, we also identified C/EBPα, a granulopoiesis-promoting transcription factor, as a substrate for CDK1. We further demonstrated that CDK1 phosphorylates C/EBPα on serine 21, which inhibits its differentiation-inducing function. Importantly, we found that inhibition of CDK1 activity relieves the differentiation block in cell lines with mutated FLT3 as well as in primary patient–derived peripheral blood samples. Clinical trials with CDK1 inhibitors are currently under way for various malignancies. Our data strongly suggest that targeting the CDK1 pathway might be applied in the treatment of FLT3ITD mutant leukemias, especially those resistant to FLT3 inhibitor therapies.
Authors
Hanna S. Radomska, Meritxell Alberich-Jordà, Britta Will, David Gonzalez, Ruud Delwel, Daniel G. Tenen
Citation Information: J Clin Invest. 2012. https://doi.org/10.1172/JCI64400.
Abstract
Cancer is principally considered a genetic disease, and numerous mutations are thought essential to drive its growth. However, the existence of genomically stable cancers and the emergence of mutations in genes that encode chromatin remodelers raise the possibility that perturbation of chromatin structure and epigenetic regulation are capable of driving cancer formation. Here we sequenced the exomes of 35 rhabdoid tumors, highly aggressive cancers of early childhood characterized by biallelic loss of SMARCB1, a subunit of the SWI/SNF chromatin remodeling complex. We identified an extremely low rate of mutation, with loss of SMARCB1 being essentially the sole recurrent event. Indeed, in 2 of the cancers there were no other identified mutations. Our results demonstrate that high mutation rates are dispensable for the genesis of cancers driven by mutation of a chromatin remodeling complex. Consequently, cancer can be a remarkably genetically simple disease.
Authors
Ryan S. Lee, Chip Stewart, Scott L. Carter, Lauren Ambrogio, Kristian Cibulskis, Carrie Sougnez, Michael S. Lawrence, Daniel Auclair, Jaume Mora, Todd R. Golub, Jaclyn A. Biegel, Gad Getz, Charles W.M. Roberts
Citation Information: J Clin Invest. 2012. https://doi.org/10.1172/JCI62888.
Abstract
Inflammatory bowel disease (IBD) is a chronic illness caused by complex interactions between genetic and environmental factors that propagate inflammation and damage to the gastrointestinal epithelium. This state of chronic inflammation increases the risk for development of colitis-associated cancer in IBD patients. Thus, the development of targeted therapeutics that can disrupt the cycle of inflammation and epithelial injury is highly attractive. However, such biological therapies, including those targeting epidermal growth factor receptor pathways, pose a risk of increasing cancer rates. Using two mouse models of colitis-associated cancer, we found that epidermal growth factor receptor inactivation accelerated the incidence and progression of colorectal tumors. By modulating inflammation and epithelial regeneration, epidermal growth factor receptor optimized the response to chronic inflammation and limited subsequent tumorigenesis. These findings provide important insights into the pathogenesis of colitis-associated cancer and suggest that epidermal growth factor–based therapies for IBD may reduce long-term cancer risk.
Authors
Philip E. Dubé, Fang Yan, Shivesh Punit, Nandini Girish, Steven J. McElroy, M. Kay Washington, D. Brent Polk



Copyright © 2024 American Society for Clinical Investigation
ISSN: 0021-9738 (print), 1558-8238 (online)